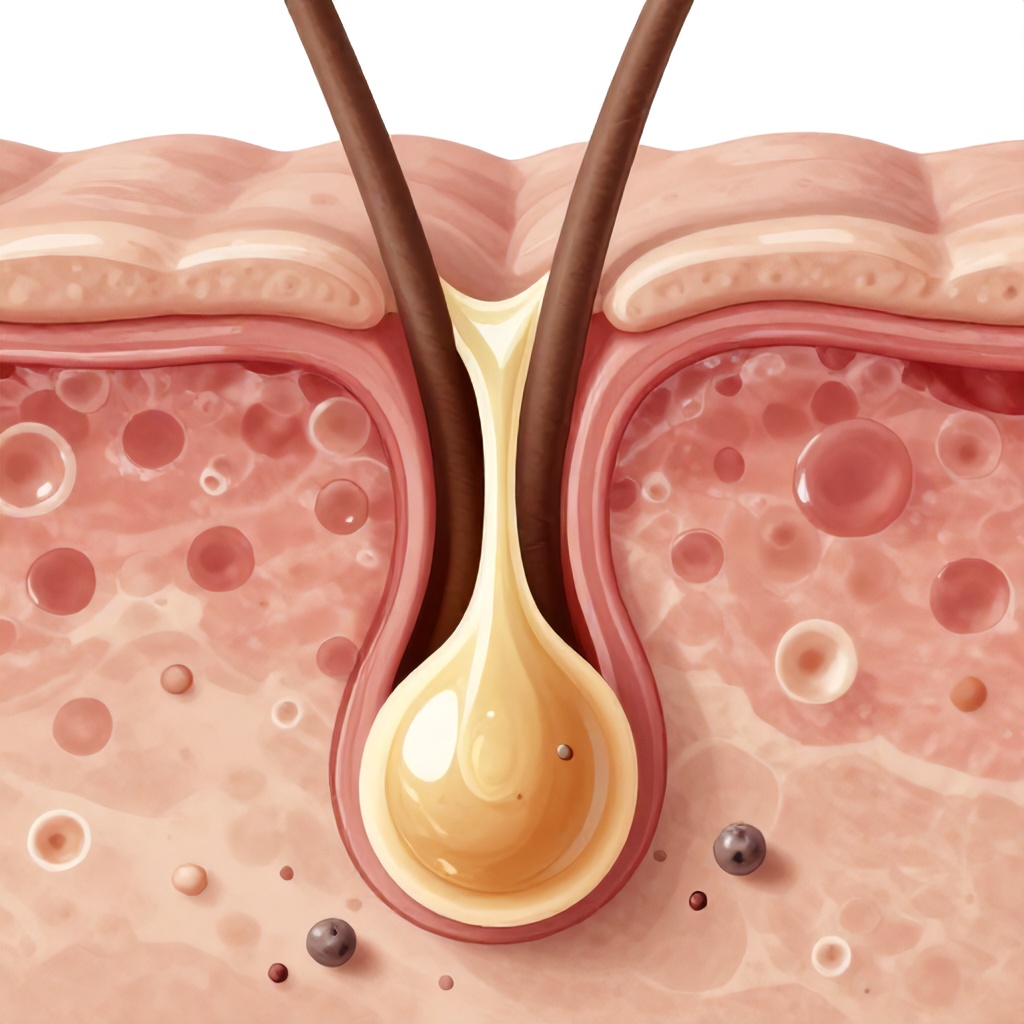
Acne is a common skin condition rooted in how our skin functions, specifically within the tiny structures called follicular units, which include our hair follicles and sebaceous glands. Understanding the biological progression of acne, from a healthy pore to various skin lesions, helps clarify why certain treatments work and how to better care for your skin.
Understanding Healthy Skin: The Foundation
Before we look at acne, it helps to understand what healthy skin looks like on a microscopic level. Your skin, the body’s largest organ, is a complex barrier made of several layers. The outermost layer is the epidermis, which protects you from the environment. Beneath that is the dermis, containing connective tissue, blood vessels, nerves, and crucially for our discussion, hair follicles and sebaceous glands.
Each hair follicle is a tiny tunnel in your skin from which hair grows. Attached to almost every hair follicle is a sebaceous gland, which produces an oily substance called sebum. Sebum is essential for keeping your skin and hair moisturized and protected. In a healthy pore, sebum flows freely up the hair follicle and onto the skin’s surface, carrying dead skin cells along with it without any issues.
The Follicular Unit and Sebum Production
The follicular unit is the core player in acne development. It’s a mini-ecosystem consisting of the hair follicle, the sebaceous gland, and the hair shaft itself. When this system is working optimally, it contributes to overall skin health. The sebaceous gland produces sebum at a balanced rate, and the lining of the pore sheds dead skin cells efficiently, preventing blockages.
The Beginnings of Acne: Non-Inflammatory Lesions
Acne often starts subtly, with what are known as non-inflammatory lesions. These are blockages in the pore that haven’t yet caused significant redness or swelling. They are the initial signs of acne stages and are often referred to collectively as comedones.
Comedones: The Initial Blockage
A comedone is essentially a clogged hair follicle. This blockage happens when dead skin cells, instead of shedding normally, mix with sebum and clump together inside the pore. This mixture creates a plug that prevents sebum from flowing out freely. This is the fundamental step in acne progression.
Whiteheads (Closed Comedones)
Whiteheads are small, flesh-colored or whitish bumps that appear on the skin. They are called “closed” comedones because the pore opening is blocked by a thin layer of skin cells. This means the trapped sebum and dead skin cells are not exposed to the air. Because they are closed off, the material inside remains soft and white, giving them their characteristic appearance. They are typically small and often don’t cause much discomfort, but they represent a significant step in the pathophysiology of acne.
Blackheads (Open Comedones)
Blackheads are small, dark spots that appear on the skin. Unlike whiteheads, the pore opening for a blackhead remains open, allowing the trapped sebum and dead skin cells to be exposed to air. The dark color isn’t dirt; it’s actually due to oxidation. When the sebum and cellular debris inside the pore react with oxygen in the air, they turn dark, much like how a cut apple turns brown. This exposure also makes them “open” comedones. Both whiteheads and blackheads are common forms of non-inflammatory acne and are crucial to recognize in any dermatological illustration of acne.
When Things Get Inflamed: Inflammatory Acne
When non-inflammatory comedones become irritated or infected, they progress to inflammatory acne. This stage involves the immune system responding to bacteria and rupture within the follicular unit, leading to redness, swelling, and pain. This marks a more advanced biological progression of acne.
The Role of Bacteria and Inflammation
Our skin naturally hosts various bacteria, including Cutibacterium acnes (formerly known as Propionibacterium acnes), or C. acnes. In a healthy pore, these bacteria exist in balance. However, when a pore becomes clogged with sebum and dead skin cells, it creates an oxygen-deprived environment that C. acnes bacteria love. They multiply rapidly, breaking down sebum into irritating fatty acids. This process, combined with pressure from the expanding plug, can cause the wall of the hair follicle to rupture. When this happens, the contents—sebum, dead skin cells, and bacteria—spill into the surrounding skin tissue, triggering an immune response. This response is what we see as inflammation: redness, swelling, and pain.
Papules: Small, Red Bumps
Papules are small, solid, red, and often tender bumps that don’t have a visible pus head. They form when the wall of a hair follicle breaks, and the body’s immune system sends inflammatory cells to the area to fight off the bacteria and clean up the debris. This causes localized inflammation and swelling, resulting in the characteristic red bump. Papules are a clear sign of inflammatory acne and represent a further step in the acne progression from simple comedones.
Pustules: Pus-Filled Lesions
Pustules are similar to papules but contain a visible collection of yellowish-white pus at their center. This pus is a mixture of dead white blood cells, bacteria, and tissue fluid, which the body has sent to fight the infection. Pustules are typically red and tender at their base, with a distinct white or yellow head. They are a common type of inflammatory acne lesion and are easily identifiable in a human skin cross-section diagram showing acne.
Nodules: Deep, Painful Lumps
Nodules are larger, solid, painful lumps that develop deep beneath the skin’s surface. They occur when the follicular wall ruptures deep within the dermis, causing a more extensive and severe inflammatory response. Unlike papules and pustules, nodules do not typically come to a head and can persist for weeks or even months. They are a more severe form of inflammatory acne and can be quite painful, often leading to scarring if not properly managed. A dermatological illustration would show these lesions extending far deeper than other acne types.
Cysts: Large, Pus-Filled Sacs
Cysts are the most severe type of acne lesion. They are large, soft, painful, pus-filled lumps that resemble boils. Cysts form when a deep rupture of the follicular wall leads to a widespread inflammatory reaction, creating a sac-like lesion filled with pus and debris. These lesions are deeply embedded in the skin, can be very tender, and almost always result in scarring. Cystic acne is a serious skin condition requiring professional medical attention to prevent permanent damage and manage the intense inflammation. The depiction of these skin lesions in a scientific diagram of acne stages highlights their depth and complexity.
Acne Types and Their Progression
Acne isn’t a single condition but rather a spectrum of skin conditions, categorized by the types and severity of the lesions present. Understanding this categorization helps in determining appropriate treatment strategies for maintaining skin health.
Categorizing Acne: Mild, Moderate, Severe
Dermatologists often classify acne into mild, moderate, or severe based on the predominant types of skin lesions and their extent:
- Mild Acne: Primarily characterized by a few whiteheads and blackheads, with occasional small papules or pustules. This stage involves mostly non-inflammatory acne.
- Moderate Acne: Features more widespread blackheads and whiteheads, along with a noticeable number of papules and pustules. Inflammation is more prominent, and there might be a few small nodules.
- Severe Acne: Defined by numerous large, painful inflammatory lesions, including many papules, pustules, nodules, and often cysts. This type of acne can cover large areas of the face, chest, or back and carries a high risk of scarring.
The Biological Progression from Healthy Pore to Severe Lesions
The journey from a healthy pore to severe acne is a continuous biological progression:
- Healthy Follicular Unit: Sebum flows freely, dead skin cells shed normally, and C. acnes bacteria are in balance.
- Microcomedone Formation: Dead skin cells and sebum begin to accumulate, forming a microscopic plug within the hair follicle, not yet visible to the naked eye. This is the very first step in acne stages.
- Non-Inflammatory Comedones (Whiteheads & Blackheads): The plug grows larger, forming visible whiteheads (closed) or blackheads (open). The environment inside the pore becomes more anaerobic, encouraging C. acnes proliferation.
- Inflammatory Lesions (Papules & Pustules): The increased bacteria and pressure from the plug cause the follicular wall to rupture, spilling contents into the surrounding skin. This triggers an immune response, leading to redness and swelling (papules). If white blood cells accumulate, a pus head forms (pustules).
- Severe Inflammatory Lesions (Nodules & Cysts): Deeper and more extensive ruptures of the follicular wall lead to larger, more painful, and persistent lesions that extend into the deeper layers of the dermis. These are the most challenging skin lesions to treat and often leave scars.
This sequence illustrates the dynamic nature of acne progression, where one type of lesion can evolve into another, often worsening over time if left untreated. A scientific diagram of acne stages would visually represent these internal changes.
Factors Contributing to Acne Progression
While the internal process of sebum and dead skin cell blockage is central, several external and internal factors can influence the development and severity of acne.
- Hormonal Fluctuations: Androgens, male hormones present in both sexes, stimulate sebaceous glands to produce more sebum, particularly during puberty, menstruation, and pregnancy. This excess sebum is a primary driver of acne.
- Genetics: A family history of acne significantly increases an individual’s likelihood of developing it, suggesting a genetic predisposition to factors like sebum production, inflammation, and follicular sensitivity.
- Diet: While direct links are still being researched, some studies suggest that high glycemic index foods and dairy products may exacerbate acne in some individuals.
- Stress: Stress doesn’t directly cause acne, but it can worsen existing breakouts by influencing hormone levels and inflammation.
- Skincare Practices: Using harsh products, over-exfoliating, or picking at blemishes can irritate the skin, disrupt its barrier, and worsen inflammation, contributing to further acne progression.
- Medications: Certain drugs, such as corticosteroids, testosterone, and lithium, can trigger or worsen acne as a side effect.
Understanding these contributing factors is part of a holistic approach to managing this common skin condition and promoting long-term skin health. The pathophysiology of acne is complex, involving a combination of these elements.
Visualizing Acne: What a Diagram Shows
A scientific diagram of acne stages provides an invaluable visual aid for understanding what’s happening beneath the surface of your skin. A clear dermatological illustration, often depicting a human skin cross-section, allows you to see the intricate details of the follicular unit and how it changes during acne development.
Such diagrams typically start with a healthy pore, showing the hair follicle, sebaceous gland, and the smooth flow of sebum. Then, they progressively illustrate the formation of a microcomedone, followed by a whitehead, where the pore opening is blocked. A blackhead diagram would show the open pore with oxidized material. Further illustrations would depict the rupture of the follicular wall, the presence of bacteria, and the resulting inflammation that characterizes papules and pustules. Finally, the diagrams would show the deeper, more extensive damage associated with nodules and cysts, highlighting the severity and depth of these skin lesions.
These visual representations are crucial because much of the acne process occurs internally, invisible to the naked eye. They help demystify the biological progression, making it easier to grasp why different treatments target specific aspects of the acne cycle, from reducing sebum to fighting bacteria or calming inflammation.
Keeping Skin Healthy
Taking care of your skin and managing acne involves a combination of consistent routines and, when necessary, professional guidance. While a diagram helps you understand the problem, practical steps help address it.
- Gentle Cleansing: Wash your face twice a day with a mild cleanser to remove excess oil and dead skin cells without stripping the skin.
- Non-Comedogenic Products: Choose makeup, moisturizers, and sunscreens labeled “non-comedogenic,” meaning they are formulated not to clog pores.
- Topical Treatments: Over-the-counter options containing salicylic acid or benzoyl peroxide can target different aspects of acne, from exfoliation to killing bacteria.
- Avoid Picking: Squeezing or picking at blemishes can worsen inflammation, push bacteria deeper into the skin, and lead to scarring.
- Professional Help: If your acne is persistent, severe, or causing distress, consult a dermatologist. They can offer prescription medications, in-office procedures, and personalized advice to manage your specific skin conditions and improve overall skin health.
Understanding the scientific diagram of acne stages, types, and progression empowers you to make informed decisions about your skincare and seek help when needed, ultimately fostering healthier, clearer skin.