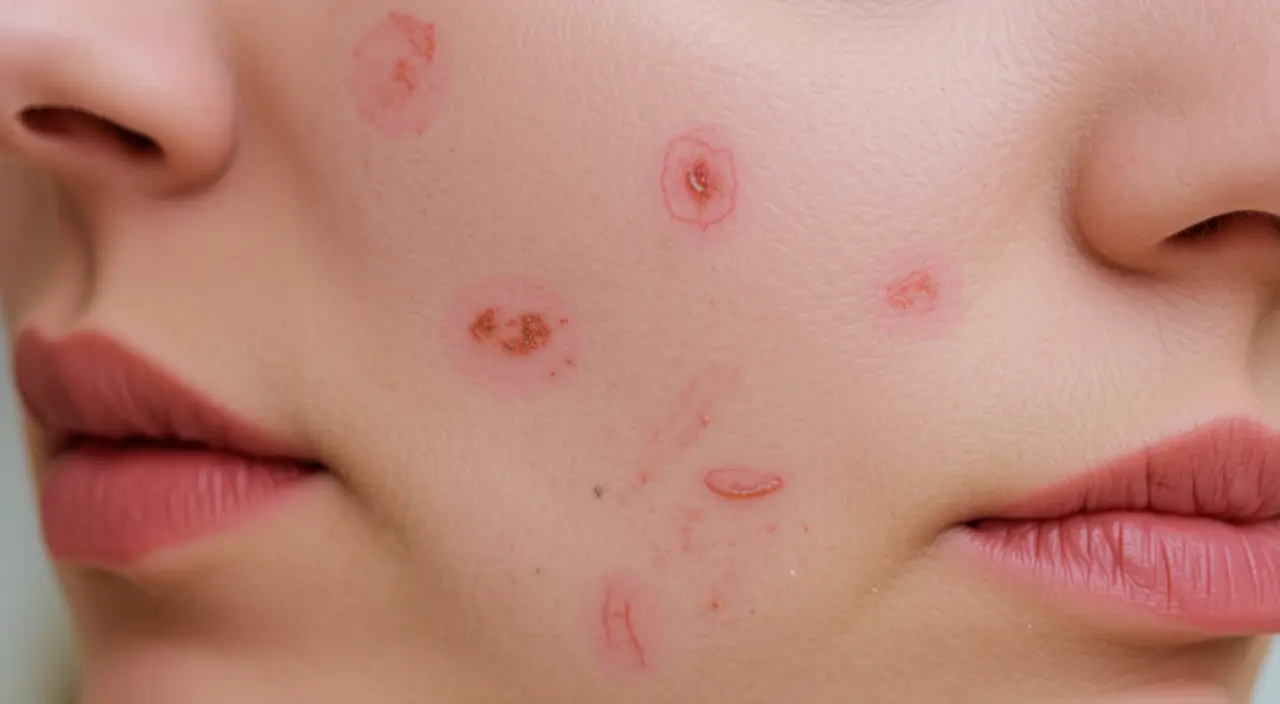
Those persistent pink or red spots left behind after an acne breakout, known as post-inflammatory erythema (PIE), are a common and often frustrating after-effect of pimples, but they are absolutely treatable and preventable with the right approach.
What is Post-Inflammatory Erythema (PIE)?
Post-inflammatory erythema, or PIE, refers to the red or purplish marks that can linger on your skin long after a pimple has healed. The term PIE itself is relatively new, coined about a decade ago to specifically describe these distinct pink, red, or purple post-acne lesions, differentiating them from other types of lingering marks on the skin.
You can think of a pimple as a tiny wound on your skin. When your body’s immune system jumps into action to fight off the acne-causing bacteria and clear the infection, it triggers skin inflammation. As this inflammation subsides and the skin begins its healing process, the small blood vessels, also known as capillaries, in the affected area can become damaged or stay dilated. This causes that telltale redness or purplish hue to show through the skin, creating what we call after-acne red spots or post-pimple marks.
These marks are most commonly associated with inflammatory breakouts, which include types of acne like papules, pustules, and cysts. This is why PIE is often referred to as post-acne erythema. While they can be quite stubborn and seem to last for months or even years, it’s important to remember that PIE is temporary and will eventually fade. This temporary nature is what sets it apart from true acne scarring, which involves changes in skin texture.
What Causes Post-Acne Erythema?
Not everyone who experiences acne will develop PIE, and the intensity of these after-acne red spots can vary significantly from person to person, and even from one pimple to the next. The primary driver behind post-inflammatory erythema is skin inflammation.
If you primarily deal with non-inflammatory acne, such as blackheads and whiteheads, you are less likely to see these pink or red marks. However, if your breakouts frequently include inflammatory papules, pustules, deeper nodules, or cysts, the chances are much higher that you’ll notice some degree of redness as these lesions heal.
Certain skin characteristics also play a role. People with fairer skin tones, typically Fitzpatrick skin types I, II, and III, tend to be more susceptible to developing post-acne erythema. This is because the redness is often more visible against lighter complexions. Similarly, individuals with naturally thinner skin may also find these marks more pronounced, as the dilated blood vessels are closer to the surface. The healing skin itself can become thinner temporarily, making the underlying vascular changes more apparent.
The degree of inflammation is key. A larger, deeper, or more irritated pimple will generally cause more significant skin inflammation than a smaller one. This increased inflammation leads to more pronounced dilation or damage of the capillaries, resulting in a more noticeable and longer-lasting PIE mark.
PIE vs. PIH: Understanding the Difference
It’s easy to confuse post-inflammatory erythema (PIE) with post-inflammatory hyperpigmentation (PIH), as both are common post-pimple marks. However, they are distinct conditions with different underlying causes and, importantly, different treatment approaches.
Post-Inflammatory Erythema (PIE)
PIE is characterized by its color: pink, red, or purplish marks. These marks are caused by damage or dilation of the tiny blood vessels (capillaries) in the skin following inflammation. When you press on a PIE mark, it often blanches, meaning it temporarily turns white or lighter, because you’re momentarily pushing the blood out of those dilated vessels. This is a key diagnostic sign.
PIE is more common in individuals with lighter skin tones and is a direct result of the vascular response to skin inflammation. It doesn’t involve an overproduction of melanin, the pigment that gives skin its color.
Post-Inflammatory Hyperpigmentation (PIH)
In contrast, PIH appears as brown, dark brown, or even black spots. These marks result from an overproduction of melanin in response to inflammation or injury. When your skin experiences inflammation (like from a pimple), it can sometimes trigger melanocytes (the cells that produce melanin) to go into overdrive, depositing excess pigment in the affected area.
PIH is more prevalent in individuals with medium to darker skin tones (Fitzpatrick skin types IV, V, and VI), although it can affect anyone. Unlike PIE, PIH marks do not blanch when pressed, as they are caused by pigment deposits, not blood vessel changes.
Understanding which type of mark you have is crucial because treatments for PIE focus on reducing redness and repairing blood vessels, while treatments for PIH target melanin production and pigment removal. Some people can, unfortunately, experience both PIE and PIH simultaneously, making the marks appear reddish-brown.
How Do You Avoid Post-Inflammatory Erythema?
Preventing PIE largely comes down to managing active acne and treating your skin gently. The less inflammation you have, the less likely you are to develop these stubborn red marks.
-
Don’t Pick or Squeeze: This is perhaps the most important rule. Picking, squeezing, or trying to pop pimples yourself significantly increases skin inflammation and the risk of damaging capillaries, leading to more severe and longer-lasting PIE. Let your breakouts heal naturally or seek professional extraction.
-
Treat Acne Early and Effectively: The best way to prevent PIE is to prevent inflammatory breakouts in the first place. Use a consistent skincare routine with ingredients designed to control acne. This might include products with salicylic acid to keep pores clear and reduce inflammation, or benzoyl peroxide to target acne-causing bacteria.
-
Be Gentle with Your Skin: Avoid harsh scrubbing, aggressive exfoliation, or using too many active ingredients at once, especially when you have active inflammatory breakouts. Treat your skin with kindness to minimize irritation and further inflammation.
-
Protect Your Skin from the Sun: Sun exposure can worsen the appearance of PIE and make it last longer. UV rays can further inflame the skin and hinder the healing process. Always use a broad-spectrum sunscreen SPF of 30 or higher, even on cloudy days, and reapply it regularly.
-
Manage Stress: Stress can trigger hormonal fluctuations that lead to increased oil production and inflammatory breakouts. Finding healthy ways to manage stress can indirectly help prevent PIE by reducing the frequency and severity of your acne.
-
Maintain a Healthy Lifestyle: A balanced diet, adequate sleep, and regular exercise all contribute to overall skin health and can help your body heal more efficiently, potentially reducing the duration and intensity of post-pimple marks.
What’s the Best Way to Treat Post-Acne Erythema?
Treating PIE requires patience and a multi-faceted approach, focusing on calming inflammation, supporting skin repair, and protecting the skin. While PIE can be stubborn, consistent treatment can significantly speed up its fading process.
Topical Treatments for PIE
Several over-the-counter ingredients can be very helpful in reducing the appearance of after-acne red spots.
-
Vitamin C Serum: This powerful antioxidant is excellent for overall skin health. It helps to brighten the complexion, supports collagen production, and can strengthen capillary walls, which may help reduce the appearance of dilated blood vessels. Look for a stable form of Vitamin C serum and apply it daily.
-
Niacinamide (Vitamin B3): Niacinamide is known for its anti-inflammatory properties. It can help calm redness, improve skin barrier function, and reduce overall skin inflammation, making it a great choice for PIE.
-
Azelaic Acid: This ingredient is a fantastic multi-tasker. It has anti-inflammatory and antibacterial properties, helps reduce redness, and can also gently exfoliate the skin. It’s often well-tolerated, even by sensitive skin types.
-
Centella Asiatica (Cica): Derived from a plant, Cica is renowned for its soothing and healing properties. It can help calm irritated skin, reduce redness, and support the skin’s natural repair processes.
-
Gentle Exfoliants (AHA/BHA): While aggressive exfoliation should be avoided, gentle use of alpha hydroxy acids (AHAs) like lactic acid or beta hydroxy acids (BHAs) like salicylic acid can be beneficial. These can help to gently resurface the skin, promoting cell turnover and allowing the red marks to fade more quickly. Salicylic acid is particularly good for continued acne prevention while also aiding in PIE fading. Always introduce them slowly and monitor your skin’s reaction.
-
Sunscreen SPF: This isn’t just for prevention; it’s a critical part of treatment. Sun exposure can darken PIE marks and prolong their healing time. A broad-spectrum sunscreen SPF 30 or higher applied daily is non-negotiable for anyone dealing with PIE.
Medicated Treatment Options
For more persistent or severe PIE, your dermatologist might recommend stronger medicated treatment options.
-
Topical Prescription Medications: Certain prescription creams or gels, such as those containing retinoids (like tretinoin or adapalene), can help accelerate cell turnover and improve overall skin texture and tone, which can aid in fading PIE. Other options might include prescription-strength azelaic acid or specific anti-inflammatory agents.
-
Oral Medications: In some cases, if acne-causing bacteria and inflammation are still a major issue, a dermatologist might prescribe oral antibiotics or other anti-inflammatory medications to get active breakouts under control, thereby preventing new PIE marks.
In-Office Procedures
When topical treatments aren’t enough, professional in-office procedures can offer more targeted and effective solutions for post-inflammatory erythema.
-
Vascular Lasers (e.g., Pulsed Dye Laser, KTP Laser): These are considered the gold standard for treating PIE. Vascular lasers specifically target the dilated blood vessels without damaging the surrounding skin. The laser energy is absorbed by the hemoglobin in the blood, heating and collapsing the capillaries, which reduces redness. Multiple sessions are usually needed for optimal results.
-
Intense Pulsed Light (IPL): Similar to lasers, IPL uses broad-spectrum light to target redness and pigmentation. It can be effective for PIE by selectively heating and destroying the dilated blood vessels. IPL can also help with some forms of post-inflammatory hyperpigmentation, making it a versatile resurfacing treatment.
-
Chemical Peels: While more commonly associated with PIH, very superficial and mild chemical peels can sometimes help with PIE by promoting skin cell turnover and improving overall skin texture, which can indirectly aid in the fading of red marks. However, caution is advised, as aggressive peels can worsen inflammation.
-
Microneedling: This procedure involves creating tiny micro-injuries in the skin to stimulate collagen production and skin regeneration. While primarily used for acne scarring, some forms of microneedling, especially with radiofrequency, can also help improve skin tone and potentially reduce redness over time by strengthening the skin’s structure.
It’s vital to consult with a dermatologist to determine the best treatment plan for your specific skin type and the severity of your PIE. They can accurately diagnose your condition and recommend the most effective and safest options.
Dr. Pimple Popper’s PIE Picks
-
Acne System: A simple 3-step routine designed for daily use to manage breakouts.
-
AHA/BHA Swipes: Resurfacing treatment pads to gently exfoliate and improve skin texture.
-
Vitamin C Serum: A daily brightener and antioxidant to support skin health.
-
Daily Moisturizer with SPF 15: A broad-spectrum sunscreen for essential daily protection.
-
Salicylic Acid Pimple Patches: Transparent medicated treatment patches for targeted breakout care.
Dr. Lee’s Last Word
Dealing with after-acne red spots can be incredibly frustrating, especially when you feel like you’ve finally conquered the active breakout. Remember that post-inflammatory erythema is a common and normal part of the healing process for inflammatory breakouts. The most crucial steps are to resist the urge to pick at your skin and to consistently protect it from the sun.
While PIE can take time to fade, incorporating targeted ingredients like Vitamin C serum, niacinamide, or azelaic acid into your routine can make a noticeable difference. For more persistent marks, don’t hesitate to seek advice from a dermatologist. They can offer professional treatments like vascular lasers that specifically target the dilated blood vessels causing the redness, significantly speeding up your journey to clearer, more even-toned skin.