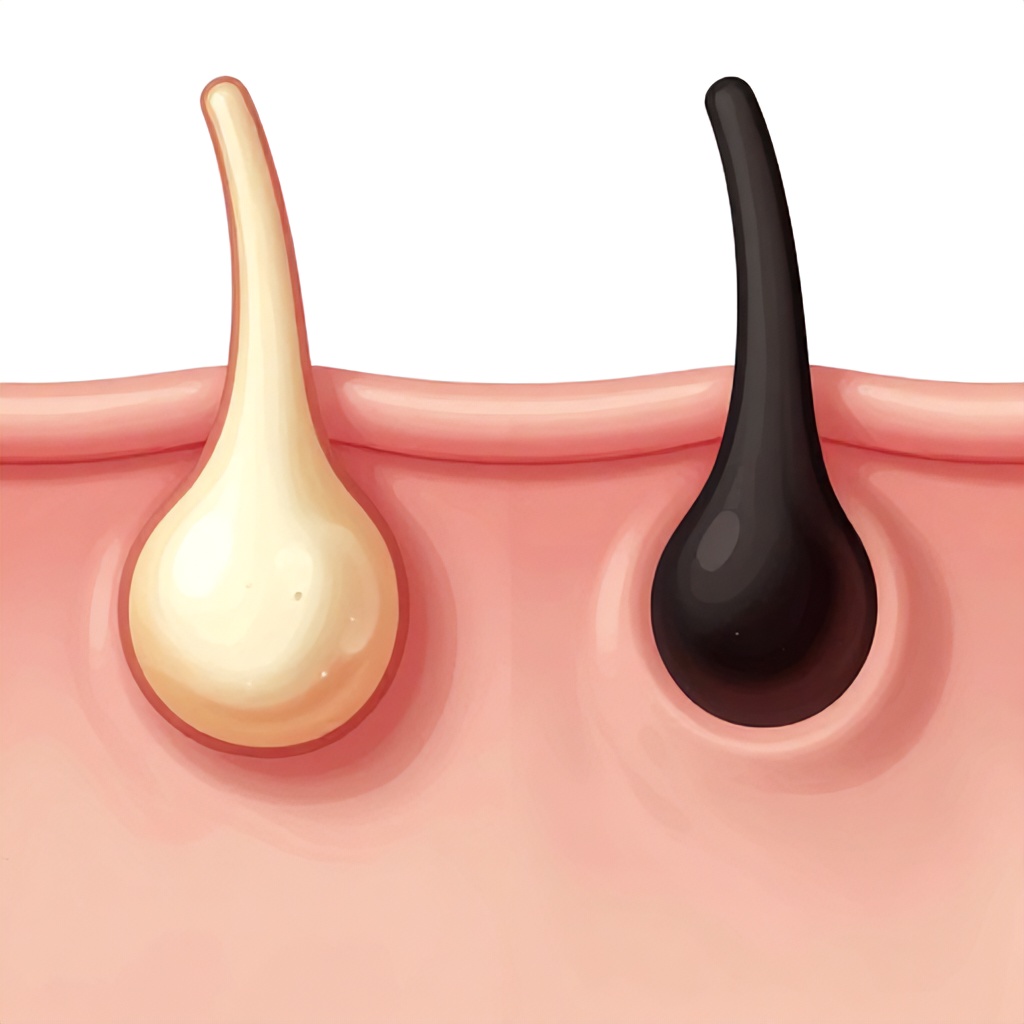
Whiteheads and blackheads are both common types of acne lesions, but they differ significantly in their appearance and formation due to whether the pore blockage is open or closed to the air.
Understanding Whiteheads
Whiteheads, medically known as closed comedones, appear as small, flesh-colored or whitish bumps on the skin’s surface. These tiny blemishes form when a hair follicle becomes completely clogged with a mixture of dead skin cells, excess oil (sebum), and sometimes bacteria. Because the pore opening is closed off from the air, the trapped material remains beneath the skin, creating a distinct white or yellowish cap.
How Whiteheads Form
The process begins deep within the pore. Our skin constantly sheds dead cells, and glands produce sebum to keep the skin moisturized. When this natural process goes awry, often due to hormonal fluctuations or an overproduction of oil, dead skin cells and sebum can accumulate. If this mixture completely blocks the pore opening, it forms a closed comedo. The material inside isn’t exposed to oxygen, which is why it maintains its pale appearance. These skin imperfections are often found on the forehead, nose, and chin, but can appear anywhere on the face or body.
Understanding Blackheads
Blackheads, or open comedones, are small, dark spots that are also a result of clogged hair follicles. Unlike whiteheads, the pore opening for a blackhead remains open to the air. This exposure is key to their characteristic dark color. When the mixture of sebum and dead skin cells in an open pore comes into contact with oxygen, it oxidizes, turning dark. It’s not dirt, as many people mistakenly believe, but rather a chemical reaction.
How Blackheads Form
Similar to whiteheads, blackheads begin with a buildup of dead skin cells and sebum within a hair follicle. However, in this case, the pore’s opening is wide enough that the trapped material is exposed to the air. The melanin (pigment) in the dead skin cells and the oxidized lipids in the sebum react with oxygen, causing the surface of the blockage to turn black or dark brown. These facial skin conditions are particularly common in the T-zone (forehead, nose, chin) where oil glands are more numerous and active.
Key Differences Between Whiteheads and Blackheads
While both are non-inflammatory acne lesions, understanding their distinct characteristics is helpful for proper skincare management. The primary distinction lies in whether the pore is open or closed.
-
Appearance: Whiteheads are small, raised, flesh-colored or white bumps. Blackheads are flat or slightly raised dark spots, resembling specks of dirt embedded in the skin.
-
Pore Opening: Whiteheads have a closed pore opening, meaning the blockage is sealed beneath the skin’s surface. Blackheads have an open pore opening, exposing the trapped material to air.
-
Color: The white color of a whitehead comes from the trapped sebum and dead skin cells not being exposed to oxygen. The dark color of a blackhead results from the oxidation of the trapped material when it comes into contact with air.
-
Texture: Whiteheads feel like a small bump under the skin. Blackheads can feel slightly rough or textured at the surface of the pore.
Recognizing these skin characteristics is the first step in choosing effective treatment guide options for these common skin blemishes.
Common Causes of Comedones
Both whiteheads and blackheads stem from similar underlying causes related to pore blockages. Understanding these factors is crucial for effective acne management and prevention of future skin imperfections.
Hormonal Fluctuations
Androgens, male hormones present in both sexes, increase during puberty, menstruation, pregnancy, and times of stress. These hormones stimulate the sebaceous glands to produce more sebum, leading to oilier skin. This excess oil is a prime ingredient for clogged pores.
Excess Sebum Production
Some individuals naturally produce more oil than others. This overproduction of sebum can overwhelm the pores’ ability to shed dead cells effectively, leading to blockages. Oily skin types are more prone to developing comedones.
Dead Skin Cell Accumulation
Our skin constantly renews itself, shedding old cells. However, sometimes these dead skin cells don’t shed properly and instead stick together, mixing with sebum to form a plug within the hair follicle. This is a direct cause of pore blockages.
Bacteria
While not the primary cause of whiteheads and blackheads themselves (which are non-inflammatory), the presence of Propionibacterium acnes (P. acnes) bacteria within clogged pores can lead to inflammation and the development of more severe pimple types, like pustules and cysts. However, the initial comedo formation is independent of bacterial infection.
Genetics
If your parents or close relatives experienced acne, you might be more genetically predisposed to developing it, including whiteheads and blackheads. Genetic factors can influence oil production, skin cell turnover, and inflammatory responses.
Certain Skincare Products
Using comedogenic skincare products, makeup, or hair products can contribute to pore blockages. These products contain ingredients that are known to clog pores, exacerbating the formation of whiteheads and blackheads. Always look for labels like “non-comedogenic” or “oil-free.”
Friction and Pressure
Constant friction or pressure on the skin, such as from tight headbands, helmets, or even leaning your face on your hands frequently, can irritate hair follicles and contribute to the development of acne lesions.
Comprehensive Treatment Guide
Treating whiteheads and blackheads involves a combination of consistent skincare practices and targeted products. The goal is to unclog pores, reduce oil production, and prevent new blemishes from forming. This section offers dermatological solutions, from over-the-counter options to professional interventions.
Daily Skincare Routine Essentials
A gentle, consistent skincare routine is the foundation for managing comedones.
-
Cleanse Gently: Wash your face twice daily with a mild, sulfate-free cleanser. Harsh scrubbing can irritate the skin and worsen breakouts. Look for cleansers containing salicylic acid for an extra boost in clearing pores.
-
Moisturize: Even oily skin needs hydration. Choose a lightweight, non-comedogenic moisturizer to prevent your skin from overcompensating by producing more oil. Hydrated skin functions better and can help with skin health.
-
Sun Protection: Many acne treatments make your skin more sensitive to the sun. Use a broad-spectrum, non-comedogenic sunscreen with at least SPF 30 every morning. Sun exposure can also worsen hyperpigmentation from past blemishes.
Over-the-Counter (OTC) Topical Treatments
These skincare products are widely available and effective for many individuals with mild to moderate whiteheads and blackheads.
-
Salicylic Acid: A beta-hydroxy acid (BHA), salicylic acid is oil-soluble, meaning it can penetrate deep into the pores to dissolve the sebum and dead skin cell plugs. It’s particularly effective for blackheads and general pore blockages. You’ll find it in cleansers, toners, and spot treatments. Start with lower concentrations (0.5-2%) to avoid irritation.
-
Benzoyl Peroxide: While primarily known for its antibacterial properties against P. acnes, benzoyl peroxide also has mild exfoliating effects that can help prevent new comedones and clear existing ones. It works by introducing oxygen into the pore, which is toxic to anaerobic bacteria. It’s available in various strengths (2.5-10%) in washes, creams, and gels. Be aware it can bleach fabrics.
-
Adapalene (Differin Gel): This is a retinoid, specifically a topical retinoid, that was once prescription-only but is now available OTC. Adapalene works by normalizing skin cell turnover and preventing dead skin cells from clogging pores. It’s highly effective for both whiteheads and blackheads and is a cornerstone of acne management. Introduce it slowly, as it can cause initial dryness and purging (a temporary increase in breakouts).
-
Alpha Hydroxy Acids (AHAs): Glycolic acid and lactic acid are AHAs that work on the skin’s surface to exfoliate dead skin cells. They can improve skin texture and help prevent pore blockages, making them useful for overall skin appearance and preventing skin imperfections. They are water-soluble and best for surface exfoliation.
Prescription Topical Treatments
For more persistent or widespread comedones, a dermatologist may prescribe stronger topical treatments.
-
Topical Retinoids (Tretinoin, Tazarotene): Stronger retinoids like tretinoin (Retin-A) and tazarotene (Tazorac) are highly effective at regulating cell turnover, preventing new comedones, and clearing existing ones. They can be more potent than adapalene and may require a period of adjustment due to potential irritation, dryness, and increased sun sensitivity. These are powerful dermatological solutions.
-
Topical Antibiotics: While not directly treating comedones, antibiotics like clindamycin or erythromycin are often prescribed in combination with retinoids or benzoyl peroxide to reduce inflammation and kill bacteria associated with more inflammatory types of acne. They are typically not used alone to avoid antibiotic resistance.
In-Office Treatments
A dermatologist can offer procedures to quickly clear existing comedones and improve overall skin health.
-
Professional Extractions: A trained dermatologist or esthetician can safely and effectively remove whiteheads and blackheads using sterile tools. Attempting to extract blemishes yourself can lead to skin damage, scarring, and infection. This is a blemish removal technique best left to professionals.
-
Chemical Peels: Light to medium chemical peels use acids (like salicylic acid, glycolic acid, or trichloroacetic acid) to exfoliate the top layers of skin. This helps to unclog pores, reduce oil, and improve skin texture, making them effective for both preventing and treating comedones.
-
Microdermabrasion: This procedure uses a device to gently exfoliate the outermost layer of skin, helping to remove dead skin cells and clear superficial pore blockages. It can improve skin appearance and make it smoother.
Prevention Strategies for Clearer Skin
Preventing whiteheads and blackheads requires a proactive approach and consistency in your skincare routine and lifestyle choices. These skin care tips are designed to keep pore blockages at bay.
-
Maintain a Consistent Skincare Routine: Regular cleansing, moisturizing, and targeted treatment with ingredients like salicylic acid or adapalene are key to preventing new comedones. Consistency is more important than using many different products at once.
-
Choose Non-Comedogenic Products: Always check labels for “non-comedogenic,” “non-acnegenic,” or “oil-free” on all your skincare products, makeup, and even hair products. This minimizes the risk of introducing pore-clogging ingredients to your skin.
-
Avoid Picking or Squeezing: Manipulating whiteheads and blackheads can push bacteria deeper into the skin, leading to inflammation, infection, scarring, and post-inflammatory hyperpigmentation. Leave extractions to professionals.
-
Clean Regularly: Regularly clean items that touch your face, such as phone screens, pillowcases, makeup brushes, and eyeglasses. These items can harbor oil, dirt, and bacteria that contribute to breakouts.
-
Shower After Sweating: If you exercise or sweat heavily, shower promptly to remove sweat, oil, and bacteria from your skin, especially on your face and body where acne can occur.
-
Consider Diet: While the link between diet and acne is complex and varies by individual, some people find that reducing high-glycemic foods (sugary snacks, refined carbohydrates) and dairy products can help improve their skin. Pay attention to how your body reacts to certain foods.
-
Manage Stress: Stress doesn’t directly cause acne, but it can trigger hormonal changes that lead to increased oil production and inflammation, potentially worsening breakouts. Incorporate stress-reducing activities into your daily routine.
When to See a Dermatologist
While many whiteheads and blackheads can be managed with OTC products and a good skincare routine, there are times when professional guidance is invaluable. If your acne is persistent, severe, or causing you distress, it’s time to consult a dermatologist.
-
Lack of Improvement: If you’ve consistently used OTC treatments for several weeks or months without seeing significant improvement in your skin blemishes.
-
Worsening Acne: If your whiteheads and blackheads are progressing to more inflammatory pimple types like cysts or nodules, which can be painful and lead to scarring.
-
Scarring or Hyperpigmentation: If you are experiencing acne scarring or dark spots (post-inflammatory hyperpigmentation) after breakouts, a dermatologist can recommend treatments to minimize these long-term effects.
-
Impact on Quality of Life: If your acne is affecting your self-esteem, causing anxiety, or impacting your daily life, a dermatologist can offer effective solutions and support.
-
Need for Prescription Treatments: A dermatologist can prescribe stronger topical or oral medications, or recommend in-office procedures that are not available over the counter.
A dermatologist can provide a personalized treatment plan, combining various approaches for optimal acne management and helping you achieve clearer, healthier skin.