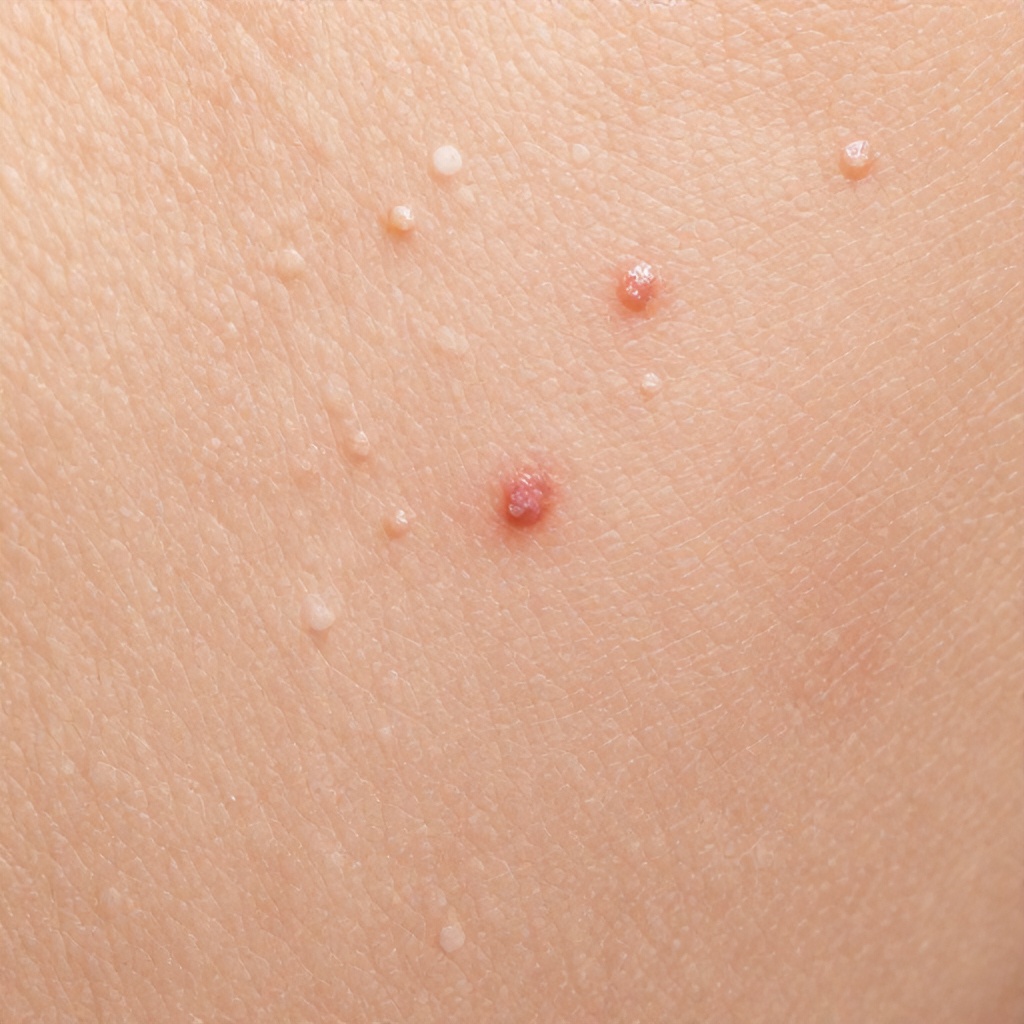
Observing a close-up of human skin often reveals a fascinating landscape, sometimes dotted with numerous small raised dermal lesions that can range from barely perceptible bumps to more prominent textural changes on the skin surface.
Understanding Small Raised Dermal Lesions on Your Skin
These small raised bumps are essentially minor changes in your skin’s topography, originating either in the epidermis, the outermost layer, or the dermis, the layer beneath it. They represent a broad category of dermatological irregularities, often benign, that contribute to the overall skin texture and appearance. A magnified view can make these micro-lesions more apparent, showcasing their distinct shapes, sizes, and colors against the surrounding skin tone.
Many individuals experience these cutaneous anomalies at some point, whether they appear as tiny, pale lesions or have a more reddish undertone. While some are fleeting, others are persistent features of the skin, reflecting various underlying biological processes or external influences. Understanding what these skin imperfections are and why they occur is the first step toward effective management and peace of mind.
Common Types of Small Raised Dermal Lesions
The variety of small raised dermal lesions is quite extensive, each with its own characteristics and typical presentation. Here are some of the most frequently encountered types:
Milia
These are tiny, pearly white or yellowish cysts, usually measuring 1-2 millimeters in diameter, that form when keratin, a protein, gets trapped under the skin’s surface. They are incredibly common, often appearing on the face, especially around the eyes and nose, but can occur anywhere. Milia are harmless and typically don’t cause any discomfort, though they can be aesthetically bothersome. They often feel like small, hard bumps.
Keratosis Pilaris (KP)
Often described as “chicken skin,” keratosis pilaris manifests as numerous small, rough bumps, typically on the upper arms, thighs, buttocks, and sometimes the face. These bumps are caused by an overproduction of keratin that clogs hair follicles, leading to small, sometimes reddish or brownish, raised areas. The skin texture in affected areas feels bumpy and dry, and the condition often worsens in dry climates or during winter months. It’s a very common, harmless genetic skin condition.
Acne Lesions (Comedones, Papules)
Acne is a widespread skin condition that results in various types of raised bumps. Whiteheads (closed comedones) are small, flesh-colored or whitish bumps that form when a hair follicle becomes clogged with oil and dead skin cells, remaining beneath the skin surface. Blackheads (open comedones) are similar but have an open pore, exposing the trapped material to air, which oxidizes and turns dark. Papules are small, red, tender bumps that lack a pus-filled head, indicating inflammation. These are all common dermatological features, particularly on the face, chest, and back, and are influenced by hormones, genetics, and bacteria.
Folliculitis
This condition involves the inflammation of hair follicles, often appearing as small, red bumps or pus-filled pimples that resemble acne. It can occur anywhere hair grows, frequently seen on the scalp, neck, chest, back, buttocks, and legs. Folliculitis is typically caused by bacterial or fungal infections, or sometimes by irritation from shaving or friction. The raised bumps can be itchy or tender.
Sebaceous Hyperplasia
These are small, flesh-colored, yellowish, or slightly reddish bumps with a central indentation, often appearing on the forehead and cheeks. They are enlarged oil glands and become more common with age, particularly in individuals with oily skin. While benign, they can sometimes be mistaken for basal cell carcinoma, making a proper diagnosis from a dermatologist important. A close-up reveals their characteristic donut-like shape.
Cherry Angiomas
Also known as senile angiomas, these are common, benign skin growths composed of small blood vessels. They appear as small, bright red, purple, or bluish raised bumps, often flat but sometimes slightly elevated. They can range from a pinhead size to several millimeters across and typically increase in number and size with age. They are particularly noticeable against lighter skin tones, like peach skin, and can have a distinct reddish undertone.
Dermatofibromas
These are firm, reddish-brown to purplish bumps that often feel like a hard nodule under the skin. They are benign fibrous growths, usually appearing on the legs but can occur anywhere. When squeezed, they often dimple inward, a characteristic known as the “dimple sign.” While typically solitary, some individuals can develop multiple dermatofibromas.
Warts
Warts are small, rough growths on the skin caused by the human papillomavirus (HPV). They can vary greatly in appearance, from flat to raised, and often have a cauliflower-like texture. Common warts frequently appear on the hands and feet, but can also be found on other parts of the body. They can be flesh-colored, white, or pink, and sometimes have tiny black dots within them, which are clotted blood vessels. Warts can be numerous and spread through direct contact.
Seborrheic Keratoses
These are common, benign skin growths that often appear as waxy, “stuck-on” looking lesions. They can be tan, brown, or black, and their texture can range from smooth to rough and crumbly. While they can be flat, many are distinctly raised, especially as they mature. They are more prevalent with age and often appear on the face, chest, back, and scalp. A magnified view often shows their irregular, sometimes greasy, surface.
Why Do These Dermal Lesions Appear? Understanding the Causes
The development of small raised dermal lesions is influenced by a complex interplay of genetic predispositions, environmental factors, and internal bodily processes. Understanding these causes can help demystify their presence on your skin.
Genetic Factors
Many skin conditions that result in small bumps have a strong genetic component. For instance, if your parents have keratosis pilaris, you are more likely to develop it. Similarly, the tendency to develop certain types of moles, skin tags, or even acne can be inherited. Your individual cellular structure and how your skin cells behave are often dictated by your genes.
Hormonal Fluctuations
Hormones play a significant role in skin health, particularly in conditions like acne. Androgens, for example, can stimulate oil glands, leading to excess sebum production that clogs pores and contributes to acne lesions. Hormonal shifts during puberty, pregnancy, or menstruation can trigger or worsen the appearance of various skin abnormalities.
Environmental Influences
Exposure to external elements is a key factor. Sun exposure, especially cumulative damage over time, can contribute to the development of seborrheic keratoses and other superficial lesions. Friction or irritation from clothing, shaving, or even vigorous scrubbing can also lead to dermatological irregularities like folliculitis or skin tags. Certain chemicals or irritants in skincare products can also provoke reactive bumps.
Inflammation and Immune Response
Many raised bumps are a manifestation of inflammation within the skin. Conditions like acne and folliculitis involve an inflammatory response to bacteria or blocked follicles. The immune system’s activity, or sometimes overactivity, can also contribute to the formation of various cutaneous anomalies.
Infections
Some small raised lesions are directly caused by infectious agents. Warts, for example, are viral in origin. Certain types of folliculitis are bacterial or fungal. Understanding the infectious nature is key to appropriate treatment, as these often require targeted antimicrobial therapies.
Aging Process
As we age, our skin undergoes numerous changes, impacting its cellular structure and overall skin topography. The prevalence of conditions like cherry angiomas, sebaceous hyperplasia, and seborrheic keratoses tends to increase with age. The skin’s ability to repair itself and maintain its barrier function diminishes, making it more susceptible to various skin imperfections.
Product Reactions and Blockages
Comedogenic ingredients in makeup or skincare products can clog pores, leading to the formation of whiteheads and blackheads. Certain ingredients can also trigger allergic reactions or irritation, resulting in small, itchy, raised bumps. Even something as simple as using too rich a moisturizer for your skin type can contribute to micro-lesions.
When to Seek Professional Advice for Skin Lesions
While many small raised dermal lesions are benign and harmless, it’s always prudent to consult a dermatologist if you have concerns. Here are specific situations where professional evaluation is particularly important:
- Any lesion that changes in size, shape, color, or texture.
- Bumps that bleed, itch persistently, or become painful.
- Lesions that appear suddenly and multiply rapidly.
- If you are unsure about the nature of a lesion.
- If you have a large number of lesions and wish to understand their cause or removal options.
- Any lesion that looks suspicious for skin cancer, especially if it’s asymmetrical, has irregular borders, varied color, or a diameter larger than a pencil eraser (the ABCDEs of melanoma).
A dermatologist can provide an accurate diagnosis, often through a close-up examination, sometimes using a dermatoscope for a microscopic view, and recommend appropriate treatment or reassurance.
Caring for Skin with Raised Lesions
Managing skin with numerous small raised dermal lesions often involves a combination of gentle care, targeted treatments, and protective measures. The goal is to improve skin texture and minimize the appearance of these dermatological features.
Gentle Cleansing
Use a mild, pH-balanced cleanser twice daily to remove dirt, oil, and makeup without stripping the skin’s natural moisture barrier. Harsh cleansers can irritate the skin, potentially worsening conditions like acne or folliculitis. For light brown skin or peach skin with reddish undertones, maintaining barrier integrity is especially important to prevent further irritation.
Thoughtful Exfoliation
Exfoliation can be beneficial for conditions like keratosis pilaris and acne by helping to unblock pores and remove dead skin cells from the epidermal surface.
- Chemical Exfoliants: Ingredients like alpha hydroxy acids (AHAs) such as glycolic or lactic acid, or beta hydroxy acids (BHAs) like salicylic acid, are excellent choices. Salicylic acid is particularly effective for oily and acne-prone skin as it penetrates oil to exfoliate within the pore.
- Physical Exfoliants: If using a physical scrub, choose one with very fine, smooth particles and use it gently to avoid micro-tears or irritation, which can exacerbate some skin abnormalities.
Always introduce new exfoliants slowly to gauge your skin’s reaction, especially if your skin tone tends to show redness easily.
Consistent Moisturizing
Keeping the skin well-hydrated is crucial, even for oily skin types. Choose a non-comedogenic moisturizer that won’t clog pores. Hydrated skin is more resilient and can better manage conditions like keratosis pilaris, where dryness can make the bumps more pronounced. For skin with pale lesions, moisturizing can improve overall skin health and appearance.
Sun Protection is Paramount
Protecting your skin from the sun is one of the most important steps for overall skin health and preventing the worsening or development of certain lesions. Use a broad-spectrum sunscreen with an SPF of 30 or higher daily, even on cloudy days. Sun exposure can darken existing lesions, contribute to new ones, and increase the risk of skin pathology.
Targeted Treatments
Depending on the specific type of raised bumps, various over-the-counter (OTC) or prescription treatments may be recommended:
- For Acne: OTC options include benzoyl peroxide and salicylic acid. Prescription treatments may include topical retinoids, antibiotics, or oral medications.
- For Keratosis Pilaris: Lotions containing urea, lactic acid, or salicylic acid can help smooth the skin.
- For Warts: OTC wart removers containing salicylic acid can be effective, but persistent warts may require cryotherapy or other treatments from a dermatologist.
- For Folliculitis: Topical or oral antibiotics or antifungals may be prescribed depending on the cause.
Always follow medical advice when using prescription treatments to address specific skin details.
Prevention and Healthy Skin Habits
Adopting a consistent and thoughtful skincare routine can significantly reduce the likelihood of developing new dermatological features and maintain the health of your skin. Regular, gentle care supports the skin’s natural barrier and resilience.
Maintaining good hygiene, especially after sweating or exercise, helps prevent conditions like folliculitis. Choosing non-comedogenic products for both skincare and makeup is a simple yet effective strategy to minimize pore blockages and subsequent acne breakouts. A balanced diet rich in antioxidants and adequate hydration also contributes to overall skin health and can influence the appearance of your skin surface, making it less prone to various skin imperfections. Remember, healthy skin is a reflection of consistent care and attention to both internal and external factors.