The journey to clearer skin from acne often involves a significant transformation, with “before and after” pictures vividly illustrating the powerful impact of consistent and appropriate acne treatment on facial skin. Understanding what to expect during this process can provide both hope and realistic expectations for anyone dealing with skin concerns related to acne.
What Acne Looks Like Before Treatment
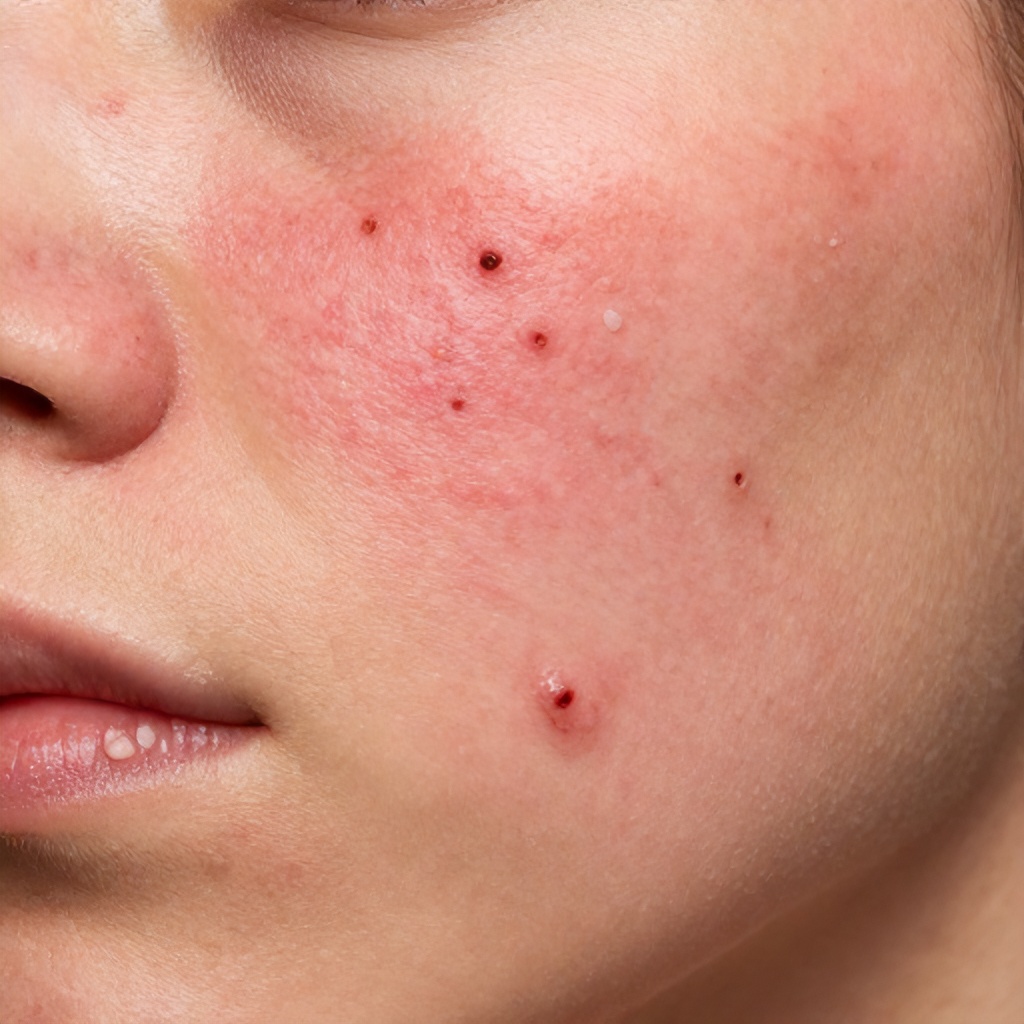
Before starting any treatment, acne presents itself in many forms, often characterized by a variety of skin blemishes and overall skin inflammation. Many individuals experience red lesions, which are often tender to the touch, alongside more prominent white pustules that signal active infection. The skin condition can also include numerous dark pores, commonly known as blackheads, and smaller, flesh-colored bumps called whiteheads, which contribute to an uneven skin texture.
This initial state of skin imperfections isn’t just about individual spots; it often involves widespread skin inflammation, leading to a generally red and irritated dermal appearance. The visible pores might appear enlarged, and the overall skin clarity is diminished. For some, the problem extends beyond superficial blemishes to deep, painful cysts and nodules, which are particularly challenging and can lead to significant discomfort and potential scarring.
Different Types of Acne and Their Appearance
Acne isn’t a single condition; it manifests in various ways, each with its own “before” look. Comedonal acne, often seen as the mildest form, is characterized by blackheads and whiteheads, giving the skin a bumpy, uneven texture without much redness. Inflammatory acne, however, involves more pronounced skin inflammation, presenting as red lesions, papules (small, red bumps), and pustules (red bumps with a white center). This type of acne can be quite visible and often causes discomfort.
Cystic and nodular acne represent the most severe forms. Here, the “before” picture includes large, painful, fluid-filled cysts and hard, deep nodules under the skin. These blemishes are often very red, deeply inflamed, and can persist for weeks or even months. They carry a high risk of permanent scarring, making early and effective acne treatment crucial for preventing long-term skin damage and promoting skin healing.
Understanding Acne Treatment
Acne treatment aims to address the root causes of breakouts, which include excess oil production, clogged pores, bacteria, and inflammation. The goal is not just to clear existing blemishes but also to prevent new ones from forming, leading to a sustained improvement in skin health and overall complexion improvement. Effective treatment can significantly reduce the severity of skin concerns and enhance skin clarity over time.
Common Treatment Approaches
The path to clearer skin is diverse, with numerous options tailored to different acne types and severities. Topical treatments are often the first line of defense, involving creams, gels, or lotions applied directly to the skin. These can contain ingredients like retinoids to unclog pores, benzoyl peroxide to kill bacteria and reduce inflammation, or salicylic acid to exfoliate and prevent blockages. For more widespread or stubborn acne, oral medications might be prescribed. These include antibiotics to reduce bacteria and inflammation, hormonal therapies for women, or isotretinoin for severe, recalcitrant acne. Each of these approaches contributes to a dermatological transformation, aiming to diminish skin imperfections and promote healthier skin.
Beyond daily applications and pills, in-office procedures can also play a vital role. Chemical peels help to exfoliate the skin and reduce breakouts. Laser and light therapies target bacteria and inflammation, improving the overall skin condition. Extractions performed by a professional can safely remove blackheads and whiteheads, preventing them from developing into more inflamed lesions. Combining these methods often yields the best treatment results, leading to more dramatic before and after differences.
The “After” Picture: What Clearer Skin Means
After successful acne treatment, the “after” picture is often one of remarkable skin transformation. The most obvious change is a significant reduction in active breakouts. The inflamed skin, red lesions, and white pustules that once dominated the facial skin begin to fade, replaced by a much calmer and more even complexion. This post-treatment skin typically shows fewer new blemishes, and existing ones heal more quickly.
The skin clarity improves dramatically. Where once there were numerous visible pores clogged with dark debris, these often appear smaller and less noticeable. The overall redness from skin inflammation subsides, revealing a more uniform skin tone. This shift from an irritated, bumpy surface to smoother skin is a hallmark of effective treatment results, signifying a significant step forward in skin health.
Beyond Just Blemishes: Improvements in Skin Texture and Tone
The benefits of effective acne treatment extend far beyond simply clearing individual spots. One of the most gratifying aspects of the “after” phase is the improvement in skin texture. The rough, uneven feel caused by persistent breakouts and underlying inflammation gives way to smoother skin. This is partly due to the reduction of active lesions and partly because many treatments encourage healthy skin cell turnover, leading to a softer, more refined surface.
Furthermore, complexion improvement is a common outcome. The overall skin tone becomes more even, with less redness and fewer dark spots (post-inflammatory hyperpigmentation) that often linger after blemishes heal. While some discoloration or scarring might require additional targeted treatments, the general dermal appearance becomes healthier and more radiant. This comprehensive skin transformation contributes significantly to a renewed sense of confidence and well-being.
Factors Influencing Treatment Results
Achieving optimal acne treatment results is a complex process influenced by several key factors. It is rarely a linear path, and understanding these elements can help set realistic expectations for your skin transformation.
Consistency is Key
Perhaps the most critical factor in seeing dramatic before and after results is unwavering consistency. Acne treatments, whether topical creams or oral medications, require regular application or intake as prescribed. Skipping doses or inconsistent use can severely hinder progress, as the active ingredients need time to work on the skin’s various issues, from reducing oil production to fighting bacteria and calming skin inflammation. Daily commitment is essential for noticeable improvements in skin clarity and texture.
Type and Severity of Acne
The initial skin condition, including the type and severity of acne, plays a huge role in how quickly and thoroughly treatment results become visible. Mild comedonal acne might respond relatively quickly to simple topical treatments, showing significant improvement in a few weeks. However, severe cystic or nodular acne, characterized by deep red lesions and widespread skin imperfections, often requires more aggressive and prolonged treatment courses, sometimes taking several months to a year to achieve substantial skin healing and clearer skin.
Individual Skin Response
Every individual’s skin is unique, and responses to acne treatment can vary widely. What works wonders for one person might have little effect or even cause irritation for another. Factors like skin sensitivity, hormonal fluctuations, and genetic predispositions can all influence how your facial skin reacts to different medications and therapies. This is why a personalized approach, often guided by a dermatologist, is crucial for finding the most effective regimen for your specific skin concerns.
Patience and Persistence
Acne treatment is a marathon, not a sprint. Significant skin transformation rarely happens overnight. It takes patience to allow treatments to work their magic and persistence to stick with a regimen even when initial progress seems slow. Many people experience an initial “purging” phase where acne might temporarily worsen before improving. Understanding this potential phase and maintaining commitment is vital for eventually seeing the desired before and after changes in your complexion improvement.
Managing Expectations and Potential Setbacks
While the goal of acne treatment is clearer, healthier skin, it is important to approach the journey with realistic expectations. The path to a complete skin transformation can have its ups and downs.
Not an Overnight Fix
It is crucial to remember that achieving clearer skin is a process that demands time. Expecting immediate results can lead to frustration and prematurely abandoning a potentially effective acne treatment. Most treatments require weeks, if not months, of consistent use before significant improvements in skin condition become apparent. The healing of inflamed skin and the reduction of red lesions take time, as does the regeneration of healthier post-treatment skin cells.
Dealing with Post-Inflammatory Hyperpigmentation (PIH) or Scarring
Even after active acne has cleared, some individuals may be left with reminders in the form of post-inflammatory hyperpigmentation (PIH) or acne scars. PIH manifests as dark spots or patches where blemishes once were, particularly common in individuals with darker skin tones. While these often fade over time, specific treatments like retinoids, vitamin C, or chemical peels can accelerate the complexion improvement. Acne scarring, on the other hand, involves changes in skin texture, such as pitted or raised marks, and may require more intensive dermatological procedures like laser resurfacing or microneedling to achieve smoother skin and further skin clarity.
Maintenance is Essential for Skin Health
Achieving clearer skin is a wonderful milestone, but maintaining it is an ongoing commitment. Acne is a chronic condition for many, and stopping treatment abruptly can lead to a relapse. A maintenance regimen, often involving milder topical treatments or occasional oral medications, is usually necessary to prevent new breakouts and preserve the improvements in skin health. This ongoing care ensures that the “after” picture remains consistent, preventing the return of visible pores, skin blemishes, and overall skin inflammation.
Real-Life Skin Transformation Stories (General Examples)
While every individual’s journey is unique, understanding common scenarios can provide insight into the potential for dermatological transformation with effective acne treatment. These examples illustrate the range of before and after results possible.
Example 1: Mild Comedonal Acne
Before treatment, someone with mild comedonal acne might present with a somewhat dull facial skin, characterized by numerous small white pustules and dark pores, particularly across the forehead and nose. The skin texture feels slightly rough, but there’s minimal redness or significant skin inflammation. After a few weeks of consistent use of a topical retinoid and salicylic acid cleanser, the “after” picture shows a much smoother skin surface. The visible pores appear smaller, and the skin clarity is significantly improved, with very few new blemishes. The overall complexion improvement is subtle yet noticeable, reflecting healthier skin.
Example 2: Moderate Inflammatory Acne
A person with moderate inflammatory acne might initially have widespread red lesions, several active white pustules, and areas of inflamed skin across their cheeks and chin. The dermal appearance is often quite red and irritated, with some existing dark spots from previous breakouts. Following a regimen that includes oral antibiotics and a benzoyl peroxide topical, the “after” transformation is more dramatic. The red lesions are significantly reduced, and new breakouts are rare. The skin inflammation has subsided, leading to a much calmer, clearer skin. While some faint dark spots might remain, the overall skin condition is vastly improved, showcasing effective treatment results and a path towards skin healing.
Example 3: Severe Cystic Acne
The “before” state for severe cystic acne is often distressing, marked by large, painful cysts and nodules deep within the facial skin, alongside numerous red lesions and significant skin inflammation. This level of skin imperfections can be physically uncomfortable and emotionally challenging. After a course of isotretinoin, often over several months, the “after” picture reveals a profound dermatological transformation. The active cysts are gone, and the skin is no longer deeply inflamed. While some scarring or redness might persist initially, the absence of active breakouts and the dramatic improvement in skin clarity and texture are undeniable. This post-treatment skin represents a major step towards long-term skin health, requiring ongoing care to manage residual concerns and maintain the clearer skin.
The Role of a Dermatologist
For anyone struggling with acne, especially moderate to severe cases, consulting a dermatologist is a crucial step towards achieving optimal acne treatment results. These skin care professionals can accurately diagnose the type and severity of your acne, identify contributing factors, and create a tailored treatment plan. They have access to a wider range of prescription-strength medications and in-office procedures that are often more effective than over-the-counter options for significant skin transformation.
A dermatologist can monitor your progress, adjust treatments as needed, and address any side effects or complications, such as post-inflammatory hyperpigmentation or scarring. Their expertise ensures that you are on the most effective path to clearer skin, guiding you through the complexities of skin healing and helping you achieve the best possible before and after outcome for your facial skin.
Maintaining Your Post-Treatment Skin
Once you’ve achieved your desired skin clarity and seen the positive before and after changes, the focus shifts to maintaining these results and preventing future breakouts. Consistent care is paramount for long-term skin health.
Consistent Skincare Routine
Adhering to a gentle, consistent skincare routine is fundamental for preserving your post-treatment skin. This typically involves cleansing twice daily with a mild, pH-balanced cleanser, followed by a non-comedogenic moisturizer to keep the skin hydrated without clogging pores. Many individuals also benefit from continuing a maintenance topical treatment, such as a mild retinoid or salicylic acid, a few times a week to keep pores clear and prevent new skin blemishes from forming. This proactive approach helps sustain smoother skin and a brighter complexion improvement.
Sun Protection
Protecting your skin from the sun is vital, especially when undergoing or maintaining acne treatment. Many acne medications can make your skin more sensitive to UV radiation, increasing the risk of sunburn and potentially worsening post-inflammatory hyperpigmentation. Daily use of a broad-spectrum sunscreen with an SPF of 30 or higher is essential. This not only protects your skin from sun damage but also helps to prevent dark spots from lingering, contributing to overall skin clarity and a more even dermal appearance.
Healthy Lifestyle
While diet and lifestyle alone may not cause acne, they can certainly influence overall skin health and potentially impact the frequency and severity of breakouts. A balanced diet rich in fruits, vegetables, and whole grains, along with adequate hydration, supports healthy skin healing and reduces systemic inflammation. Managing stress through practices like meditation or exercise can also be beneficial, as stress is known to exacerbate skin concerns for many. Prioritizing sufficient sleep further aids in skin repair and regeneration, contributing to a vibrant, clearer skin and helping to maintain the impressive before and after results you’ve worked hard to achieve.