Understanding Inflammatory Acne and Skin Redness
Inflammatory acne is a specific dermatological condition characterized by red, swollen, and often painful bumps that require a targeted approach to reduce skin irritation and long-term scarring. Unlike simple blackheads or whiteheads, this type of acne involves an active immune response deep within the pores. When a pore becomes blocked by excess oil and dead skin cells, bacteria known as Cutibacterium acnes can multiply. This triggers the body to send white blood cells to the area, resulting in the visible swelling and heat known as skin inflammation. For many young women, this appears as a cluster of blemishes across the cheeks or along the jawline, often creating a facial profile that feels tender and looks noticeably flushed.

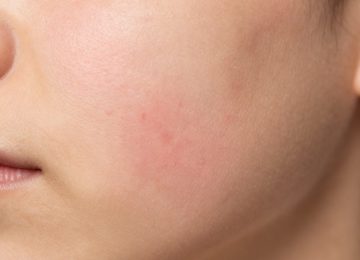
The redness associated with these breakouts is technically called erythema. It happens because the blood vessels near the surface of the skin dilate to help the healing process. While this is a natural response, it can lead to a persistent pink or purple hue even after the blemish itself has flattened. This is often referred to as post-inflammatory erythema. Managing this requires a balance between fighting the bacteria and soothing the skin barrier. If the approach is too aggressive, the redness can actually worsen, leading to increased sensitivity and a cycle of facial congestion that feels impossible to break.
Identifying Different Types of Blemishes
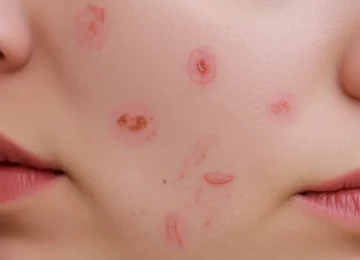
Not all spots are the same. Inflammatory acne typically presents as papules and pustules. Papules are small, firm, red bumps that do not have a visible center of pus. They feel like hard knots under the skin. Pustules are similar but feature a white or yellow dot at the tip, indicating that the body is processing the infection. In more severe cases, a person might experience nodules or cysts, which are larger, deeper, and much more painful. These deeper lesions are more likely to affect the overall skin texture and may require a professional dermatological assessment to prevent permanent indentations or scarring.
When looking at a macro skin shot of inflammatory acne, the skin texture often appears shiny or stretched over the bumps. There might be visible flaking around the edges of a blemish where the skin is trying to shed. This combination of oiliness and dryness is a common struggle for those with acne-prone skin. It indicates that the moisture barrier is compromised. A healthy barrier keeps moisture in and irritants out. When it is broken, even gentle products might cause a stinging sensation. This is why identifying the specific types of blemishes on your face is the first step toward a clearer skin journey.
Common Causes of Cheek and Jawline Breakouts
Hormonal fluctuations play a massive role in where acne appears on the face. For many women, jawline acne is a classic sign of androgen sensitivity. Androgens are hormones that can stimulate the oil glands to produce more sebum than necessary. This excess oil gets trapped in the follicles, leading to the deep, painful bumps often seen in a facial profile. These breakouts frequently flare up during specific times of the menstrual cycle, making them feel predictable yet frustrating. Stress also contributes by increasing cortisol levels, which further signals the skin to produce more oil.
Cheek breakouts can sometimes be linked to external factors. Think about what touches your face. Cell phones, pillowcases, and even your hair can carry bacteria and old makeup residue. This is often called acne mechanica, where physical friction or contact triggers a breakout. If you notice that one side of your face has more skin imperfections than the other, consider your daily habits. Do you lean your face on your hand while studying? Do you sleep on one side more than the other? These small actions can lead to localized skin irritation and clogged pores in very specific areas.
The Role of the Skin Barrier
The skin barrier is the outermost layer of your epidermis. It acts as a shield. When you have inflammatory acne, this shield is often under attack. Many people try to “dry out” their acne using harsh alcohols or scrubbing. This is a mistake. Stripping the skin of its natural oils causes the barrier to crack. This allows more bacteria to enter and more moisture to escape, a process called transepidermal water loss. The result is skin that looks red, feels tight, and produces even more oil to compensate for the dryness. This creates a vicious cycle of facial congestion and inflammation.
To support the barrier, you need ingredients that mimic the skin’s natural fats. Look for ceramides, fatty acids, and cholesterol in your moisturizers. These help to “glue” the skin cells back together. When the barrier is strong, the skin is better at defending itself against the bacteria that cause acne vulgaris. A calm barrier also means less overall skin redness. It allows the topical treatment area to heal without becoming overly dry or flaky. Rebuilding this layer is just as important as treating the actual spots.
Effective Ingredients for Inflammatory Acne
Choosing the right ingredients can feel overwhelming, but a few have stood the test of time for reducing inflammation and clearing pores. Salicylic acid is a favorite for many because it is oil-soluble. This means it can get deep into the pores to dissolve the “glue” holding dead skin cells together. It also has natural anti-inflammatory properties, which helps with the redness of papules. Benzoyl peroxide is another heavy hitter. It works by introducing oxygen into the pores, which kills the anaerobic bacteria responsible for acne. However, it can be drying, so it is best used as a spot treatment or in a low-percentage wash.
Niacinamide, also known as Vitamin B3, is excellent for sensitive skin. It helps to regulate oil production and visibly reduces the appearance of enlarged pores. Most importantly for those with skin redness, it strengthens the barrier and fades the red marks left behind after a breakout. Azelaic acid is another underrated hero. It is a gentle dicarboxylic acid that targets both the bacteria and the pigment-producing cells. It is often prescribed for rosacea because it is so good at calming erythema. Using these ingredients consistently is better than using them in high concentrations all at once.
- Salicylic Acid: Clears clogged pores and reduces swelling.
- Benzoyl Peroxide: Kills acne-causing bacteria.
- Niacinamide: Calms redness and supports the skin barrier.
- Azelaic Acid: Reduces redness and prevents dark spots.
- Adapalene: A retinoid that regulates cell turnover to prevent new clogs.
Ingredients to Use with Caution
While some ingredients help, others can make inflammatory acne much worse. Avoid heavy oils like coconut oil if you are prone to clogged pores, as these are highly comedogenic. Fragrances and essential oils like lemon or peppermint can also be major triggers for skin irritation. Even if they smell nice, they contain volatile compounds that can sensitize the skin over time. Physical scrubs with large, jagged particles—like crushed walnut shells—can create micro-tears in the skin. These tears allow bacteria to spread and increase the overall level of skin inflammation. Stick to chemical exfoliants or very soft cloths instead.
Alcohol-based toners are another common culprit. They provide a temporary “clean” feeling but ultimately dehydrate the skin. This leads to more redness and can make the skin texture look rough and dull. If a product makes your face feel “squeaky clean,” it is probably too harsh. Your skin should feel soft and hydrated after cleansing, not tight or parched. Always check the ingredient list for “alcohol denat” or “isopropyl alcohol” near the top of the list, as these are the most drying types.
Daily Routine for Calm, Clear Skin
A consistent routine is the foundation of any clear skin journey. In the morning, the goal is protection and hydration. Start with a gentle, non-foaming cleanser to remove any sweat from the night. Follow this with a hydrating serum or a niacinamide treatment. The most vital step is sunscreen. UV rays can make skin redness much worse and cause acne marks to turn into permanent dark spots. Look for a mineral sunscreen with zinc oxide, as zinc is naturally soothing for inflamed skin. Many modern formulas are lightweight and won’t contribute to facial congestion.
- Cleanse with a gentle, pH-balanced wash.
- Apply a soothing treatment like azelaic acid or niacinamide.
- Moisturize with a lightweight, oil-free lotion.
- Protect with an SPF of 30 or higher.
The evening routine is where you focus on treatment and repair. If you wear makeup or sunscreen, consider double cleansing. Use an oil-based balm or micellar water first to break down the surface debris, then follow with your regular cleanser. This ensures that your pores are truly clean before you apply active ingredients. This is the time to use your retinoid or benzoyl peroxide treatment. Finish with a slightly richer moisturizer to support the skin’s natural repair process while you sleep. Rest is when your body does the most work to heal those painful pustules and papules.
- Double cleanse to remove makeup and pollution.
- Apply your primary acne treatment (retinoid or spot treatment).
- Wait a few minutes for the product to absorb.
- Apply a barrier-repairing moisturizer with ceramides.
Lifestyle Factors and Skin Health
What you do outside of your bathroom also affects your skin. Diet is a frequent topic of debate, but some evidence suggests that high-glycemic foods—like sugary snacks and white bread—can spike insulin and trigger oil production. Some people also find that dairy contributes to their jawline acne. It can be helpful to keep a skin diary for a few weeks to see if there are any patterns between what you eat and how your skin looks. However, don’t restrict your diet too much without professional advice, as stress over food can also cause breakouts.
Sleep hygiene is another simple way to manage skin imperfections. Change your pillowcase every few days to prevent the buildup of oils and bacteria. Silk or satin pillowcases are often gentler on sensitive skin and cause less friction than cotton. Also, try to keep your hands away from your face during the day. Picking at a blemish might feel satisfying in the moment, but it pushes bacteria deeper into the pore and almost guarantees a scar. If you struggle with the urge to pick, try using hydrocolloid patches. These “pimple patches” protect the area and help draw out fluid while keeping the wound clean.
When to Seek a Dermatological Assessment
If your acne is painful, leaves scars, or doesn’t respond to over-the-counter treatments after six to eight weeks, it is time to see a professional. A dermatological assessment can provide clarity on whether your condition is standard acne vulgaris or something else, like rosacea or perioral dermatitis. A dermatologist can prescribe stronger topical treatments or oral medications that target the root cause of the inflammation. They can also offer medical aesthetics treatments, such as light therapy or chemical peels, which can speed up the healing of skin redness and improve skin texture more quickly than at-home products alone.
Professional help is especially important for deep nodules or cysts. These cannot be treated with surface-level creams. Sometimes, a dermatologist can provide a localized injection to reduce swelling quickly and prevent a scar from forming. Don’t feel like you have to “tough it out” or wait until the acne is severe to ask for help. Early intervention is the best way to ensure your clear skin journey is successful and that your skin remains healthy for years to come. Your skin is an organ, and treating it with medical expertise is a form of self-care.
Dos and Don’ts for Inflammatory Acne
Managing red, inflamed skin requires a “less is more” mindset. It is tempting to throw every product at your face, but this usually leads to more skin irritation. Focus on calming the heat first. If a blemish is particularly painful, you can apply a cold compress for a few minutes to constrict the blood vessels and reduce the throbbing sensation. This doesn’t cure the acne, but it makes the erythema less intense and provides temporary relief. Always be patient; skin cells take about a month to renew, so you won’t see the full effect of a new routine overnight.
Quick Guidance List
- Do: Use lukewarm water when washing your face. Hot water strips oils and increases redness.
- Don’t: Use “natural” remedies like toothpaste or lemon juice on spots. These are highly irritating.
- Do: Patch test new products on your neck or inner arm before applying them to your whole face.
- Don’t: Over-exfoliate. Once or twice a week is plenty for most acne-prone skin types.
- Do: Clean your makeup brushes weekly to avoid spreading bacteria.
- Don’t: Skip moisturizer. Even oily skin needs hydration to stay balanced.
The path to managing inflammatory acne is rarely a straight line. There will be days when your skin feels calm and days when a new flare-up appears. This is normal. By focusing on gentle cleansing, targeted active ingredients, and barrier protection, you can reduce the frequency and severity of these breakouts. Remember that a facial profile with some texture or redness is not a failure; it is just a sign that your skin is working hard to protect you. With the right tools and a bit of patience, the redness will fade, and your skin will find its balance again.